Originally published: May 2026 | Reviewed by Dr. Michael Berglass
What Happens If a Dental Implant Fails?
A failed dental implant is an implant that loses its bond with the jawbone, becomes mobile, or develops an infection severe enough to compromise the surrounding bone, making the implant unable to support the crown, bridge, or denture it was placed to anchor.
According to the American Academy of Implant Dentistry, dental implant failure occurs when the implant fails to integrate properly with or remain stable in the jawbone. Dental implants carry a strong clinical track record, but failure does occur.
Extensive studies show dental implants have a 90–96% success rate, with failure rates ranging from 4–10% overall.
Dr. Michael Berglass, D.D.S., of Boynton Implant and Cosmetic Dentistry in Boynton Beach, Florida, evaluates implant complications and failed implants from other providers at 2415 Quantum Blvd — at no charge for the initial consultation.
Experiencing pain, looseness, or swelling around a dental implant? Dr. Berglass evaluates implant complications at no charge — call 561-736-1700 or schedule a consultation at Boynton Implant and Cosmetic Dentistry today.
A failing dental implant produces recognizable clinical signs that distinguish implant complications from normal post-surgical recovery. Normal soreness after implant placement fades within a few days. Pain that persists beyond two weeks, worsens over time, or returns after a period of comfort signals a problem that requires evaluation of implant complications.
Persistent pain or discomfort, a loose or shifting implant, and swollen or bleeding gums are the primary warning signs of a failing implant. Movement indicates poor osseointegration or bone loss around the implant.
Swelling that persists or worsens beyond the initial healing period may indicate peri-implantitis — an infection affecting the gums and bone surrounding the implant.
Additional warning signs include gum recession that exposes the implant surface, difficulty chewing on the side of the implant, and a visible gap between the implant crown and the gumline.
Patients who notice any of these signs should contact Boynton Implant and Cosmetic Dentistry immediately rather than waiting for a scheduled appointment.
If you’re ready to get started, call us now!
Dental implant failure is divided into two clinically distinct categories based on when failure occurs and what causes it. Understanding the category helps determine the appropriate treatment response.
Early implant failure occurs when the implant fails to bond with the bone due to infection, poor bone quality, or surgical issues, with pain, bleeding, and swelling appearing shortly after the procedure.
Late implant failure results from peri-implantitis, gradual bone loss, or excessive pressure from chewing or grinding, with symptoms developing slowly over months or years.
Early failures account for roughly 83% of all implant failures, with the critical window being the osseointegration phase — the period during which the titanium post should be fusing with the surrounding jawbone. Late failures are less common but more complex to treat because bone loss has progressed before the problem becomes symptomatic.
Patients with existing implants placed elsewhere who notice late-stage symptoms can request an implant health review at dental implant aftercare.
Dental implant failure has identifiable, documentable causes — most of which can be assessed and mitigated before placement through a thorough candidacy evaluation.
Peri-implantitis is the leading cause of late implant failure. Peri-implantitis is a plaque-associated pathological condition characterized by inflammation of the tissue surrounding the implant and consequent gradual bone loss. It often goes undiagnosed in its early stages because the implant itself has no nerves to signal pain.
Bacteria accumulate around the implant post and gumline, triggering an inflammatory response that progressively destroys the bone anchoring the implant.
Smoking dramatically increases failure risk at both early and late stages. A meta-analysis of 35,118 implants published in PLOS ONE found that smoking is associated with a relative risk of 1.92 for implant failure — approximately 92% higher than that of non-smokers.
Dr. Berglass reviews smoking history as part of every candidacy evaluation to determine whether cessation protocols are warranted before implant surgery.
Uncontrolled diabetes impairs bone healing at the cellular level. Research published by the National Institutes of Health confirms that hyperglycemia can reduce bone recovery by 40% following the surgical osteotomy that implant placement requires, with bone healing deterioration correlating directly with poor glycemic control.
Patients with well-controlled diabetes — hemoglobin A1C of 7% or below — can achieve osseointegration rates comparable to patients without diabetes. Patients with diabetes are evaluated using the protocol described in the diabetes implant protocol.
Insufficient bone density prevents the implant from achieving the primary stability required for osseointegration. A 2025 retrospective analysis published in PMC identified lack of osseointegration as the cause of 36.4% of implant failures and absence of primary stability as the cause of 22.4% — together accounting for nearly 60% of all failures studied.
Patients who lack adequate bone volume require bone grafting or a sinus lift before placement — preparatory procedures that a CBCT scan identifies before any fee is committed.
Bruxism — teeth grinding — applies excessive mechanical force to the implant post and crown, disrupting osseointegration during healing and accelerating bone loss around integrated implants.
A 2024 retrospective study published in the Journal of Clinical Medicine (PMC11700303) identified bruxism and peri-implantitis as principal contributors to implant failure, with statistical significance at p=0.001.
Patients with a bruxism history require a nightguard protocol before and after implant placement to protect the investment.
If you’re ready to get started, call us now!
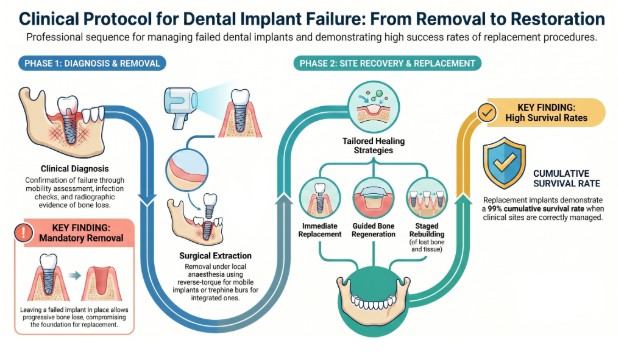
A failed dental implant follows a predictable clinical sequence once the failure is confirmed.
The treating dentist performs a clinical examination, takes updated X-rays or a CBCT scan, and assesses bone levels, mobility, and infection status around the implant. Mobility, edema, discomfort, pus, bleeding, and radiographic evidence of peri-implant bone loss are the clinical indicators used to confirm failure and determine whether the implant requires immediate removal.
Treating a failed dental implant always involves extracting the implant — leaving a failed implant in place allows progressive bone loss that reduces the available foundation for any future replacement.
The dentist performs the removal under local anesthesia. An implant with significant mobility can often be removed using a reverse-torque technique. Implants with no mobility but confirmed bone loss require surgical removal with a trephine bur.
Following removal, the treatment options include immediate replacement with a wider-diameter implant, simultaneous replacement with a guided bone regeneration procedure, or a staged approach in which lost bone and tissue are rebuilt before a new implant is placed.
The appropriate approach depends on the amount of bone remaining, the cause of the original failure, and whether infection is present at the extraction site.
A retrospective study of 381 replacement implants placed in sites where the original implant failed due to peri-implantitis found a cumulative survival rate of 99% after a mean follow-up of 34 months, with marginal bone loss of only 0.1mm.
A failed implant does not permanently preclude a successful replacement when the site is managed correctly.
Ready to have a failed or failing implant evaluated? Dr. Berglass reviews implant complications from other providers at no charge. Call 561-736-1700 or book an evaluation at 2415 Quantum Blvd, Boynton Beach.
A failed dental implant can usually be replaced once the extraction site has healed and bone volume has been restored. The candidacy criteria for replacement are the same as for first-time placement — adequate bone density, controlled systemic conditions, and healthy gum tissue — but the timeline and preparation requirements depend on the cause of the original failure.
Patients whose first implant failed due to insufficient bone typically require a bone grafting procedure before replacement.
Patients whose failure was caused by peri-implantitis require confirmed resolution of infection and demonstrated improvement in oral hygiene before a new implant is placed. Patients whose failure was smoking-related benefit most from a structured cessation protocol before the replacement procedure.
The reconstruction checklist outlines the preparatory steps that apply to complex replacement cases. Patients with questions about whether their specific situation qualifies for replacement can review implant candidacy barriers before their consultation.
Dental implant failure is not random. The leading causes — peri-implantitis, smoking, uncontrolled systemic conditions, and inadequate bone preparation — are all identifiable and addressable before placement begins.
A thorough pre-surgical evaluation using a CBCT scan confirms bone volume and density before any surgical commitment. Patients with insufficient bone receive bone grafting or a sinus lift to build sufficient bone volume before placement.
Patients with diabetes, osteoporosis, or a bisphosphonate medication history undergo a modified protocol designed to account for their specific healing profile. The preventive steps that protect long-term implant health are detailed in the implant longevity tips.
Post-placement maintenance is equally critical. Regular dental exams with imaging allow the dental team to track bone levels around the implant and detect changes before they become critical — because early implant failure typically becomes apparent within the first three to four months, during the osseointegration phase.
Patients at Boynton Implant and Cosmetic Dentistry receive a structured aftercare protocol that includes scheduled imaging reviews to catch peri-implant bone changes before they reach the threshold of failure.
What are the signs that a dental implant is failing?
The signs that a dental implant is failing include persistent or worsening pain beyond two weeks after placement, a loose or shifting implant, swollen or bleeding gums that do not resolve, gum recession that exposes the implant surface, and difficulty chewing on the side of the implant. Any of these signs warrants immediate clinical evaluation.
Can a failed dental implant be replaced?
Yes. A failed dental implant can be replaced in most patients once the extraction site has healed and bone volume has been restored. A retrospective study of 381 replacement implants found a cumulative survival rate of 99% after a mean follow-up of 34 months. The timeline and preparation required for replacement depend on the cause and severity of the original failure.
How common is dental implant failure?
Dental implant failure rates range from 4–10% based on extensive studies covering thousands of implants. Early failures — those occurring during the osseointegration phase — account for roughly 83% of all failures. Late failures caused by peri-implantitis or bone loss are less common but more complex to treat due to progressive bone deterioration before symptoms appear.
What causes dental implants to fail?
The leading causes of dental implant failure are peri-implantitis, smoking, uncontrolled diabetes, insufficient bone density, and bruxism. A 2025 PMC retrospective analysis found that a lack of osseointegration accounted for 36.4% of failures. Smoking increases failure risk approximately 92% above that of non-smokers, and uncontrolled hyperglycemia reduces bone recovery by up to 40%.
What happens when a dental implant is removed?
When a dental implant is removed, the site is evaluated for remaining bone volume and infection status. Depending on those findings, the treatment pathway is either immediate replacement with a wider-diameter implant, simultaneous replacement with guided bone regeneration, or a staged approach in which bone is rebuilt first, and the replacement implant is placed after site healing.
Does smoking cause dental implants to fail?
Smoking is a statistically significant cause of dental implant failure at both early and late stages. A meta-analysis published in PLOS ONE covering 35,118 implants found a relative risk of 1.92 for failure in smokers compared to non-smokers. Tobacco directly inhibits osteoblast function, slows healing, and increases susceptibility to peri-implantitis.
How long does it take to replace a failed dental implant?
Replacing a failed dental implant typically takes three to twelve months from removal to final restoration, depending on the extent of bone loss and the preparatory procedures required. Patients with adequate remaining bone and no active infection may qualify for earlier replacement. Patients requiring bone grafting or guided bone regeneration need additional healing time before a new implant can be placed.
How does Dr. Berglass evaluate failed implants from other providers?
Dr. Berglass evaluates failed implants placed by other providers using a CBCT scan, clinical examination, and review of the patient’s medical and dental history. The evaluation identifies bone loss extent, infection status, and the cause of the original failure — and produces a written treatment plan covering removal, site preparation, and replacement options before any procedure begins.
A failed implant is not the end of the road. Dr. Berglass at Boynton Implant and Cosmetic Dentistry evaluates and treats failed implants from any provider — request your evaluation or call 561-736-1700.
Reason To Smile

Phone
Address
2415 Quantum Blvd
Boynton Beach, FL 3342
Office Hours
Mon - Thurs: 8:30AM-5PM
Fri: 8:30AM-1PM
Sat - Sun: Closed